What is a cataract?
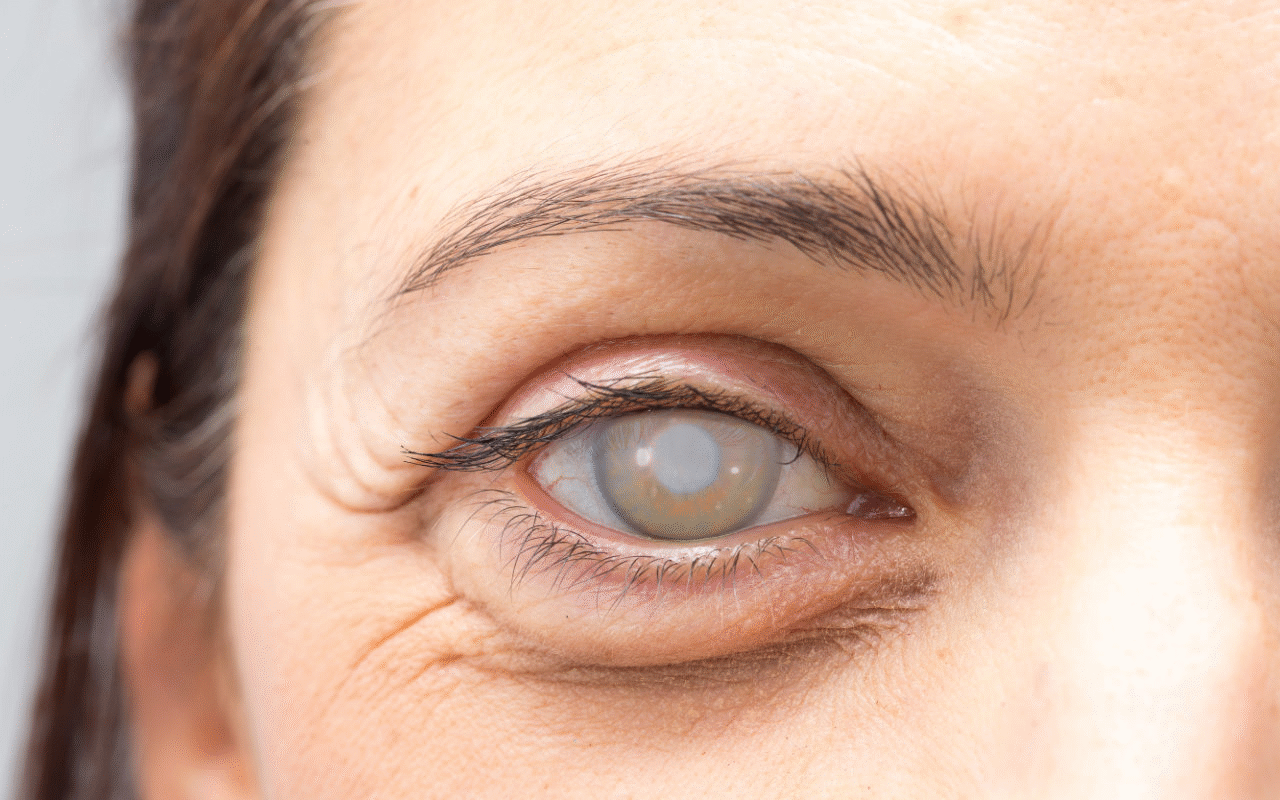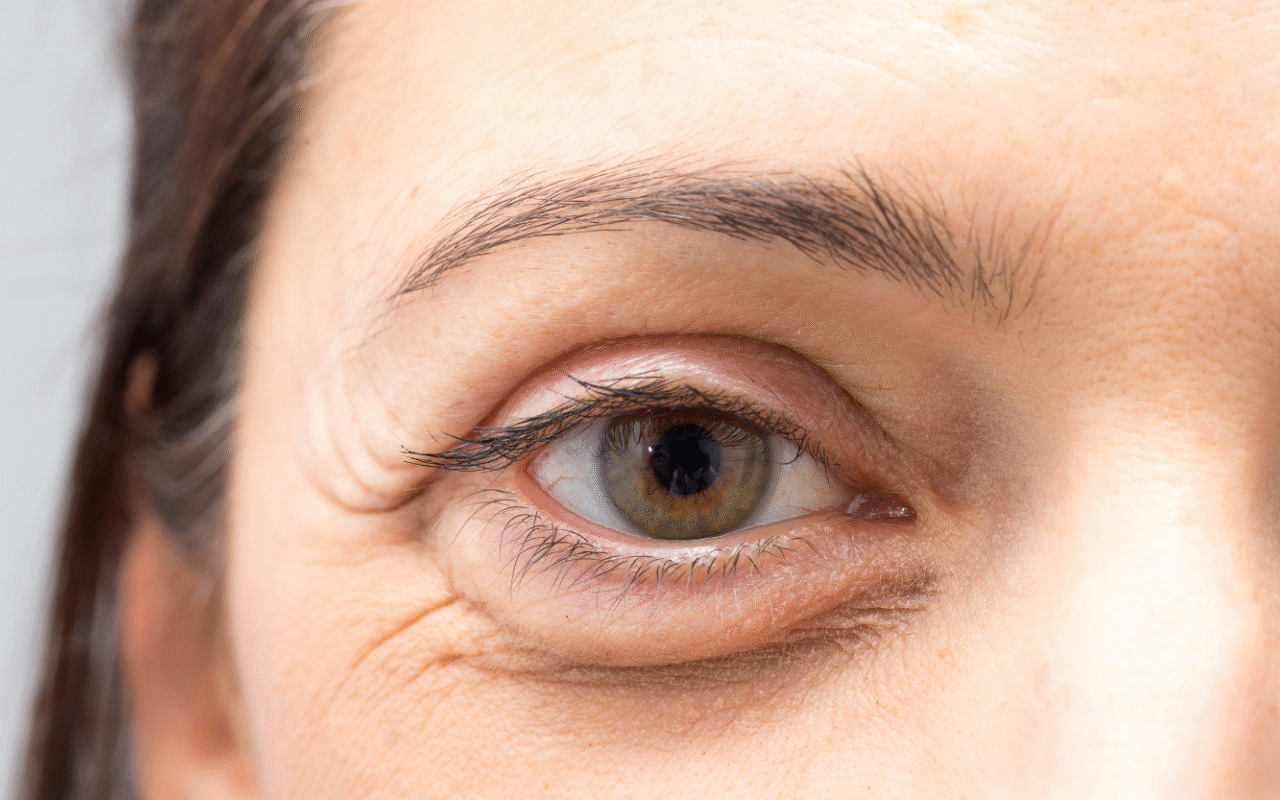
The clouding of the eye's natural lens
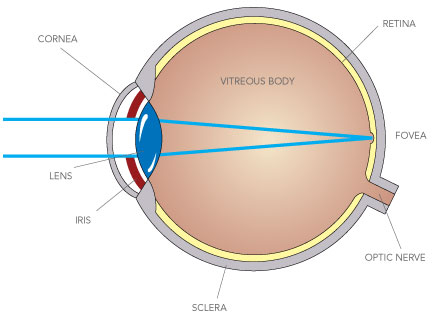
The best way to understand a cataract is to have brief understanding of the structure of the eye. The diagram shows the structure of the eye.
The front of the eye is covered by clear structures i.e. the cornea and the crystalline lens, which together bring the image to a sharp focus on the retina, which lines the inside of the back of the eye.
The best way is to think of the eye is as a cinema, where the cornea and the lens are the projectors and the flat retina on which the image is focused is the cinema screen.
Whilst the cornea has a fixed curvature and shape, the lens is able to change its shape to bring objects of different distances to a sharp focus on the retina. A cataract is a condition where the lens of the eye loses its clarity and thus either prohibits light from passing through or misdirects light rays, thereby interfering with the projection of a bright and sharp image on the retina.
What is the treatment for cataracts?
The only definitive treatment for cataract is exchanging the lens of the eye with an artificial lens implant. This is what is referred to as cataract surgery or cataract extraction. Occasionally when symptoms are very mild you may find that spectacles temporarily resolve the symptoms.
Do I need to have cataract surgery, if I have a cataract?
No. The final visual outcome is not dependent on the time of intervention. The most important factor determining the need for surgery is whether or not you are troubled by your visual symptoms. If you are satisfied with your level of vision, then you do not need to have cataract surgery just because you have a cataract and you are free to defer the option of surgery.
There are however exceptions where cataract surgery is recommended even though you may not wish to have surgery or are not troubled by your vision. These are:
a) If your vision does not meet the legal minimum requirements for driving and you wish to continue to drive.
b) If the cataract prohibits an adequate view to enable monitoring or treating the back of the eye (retina), for example in diabetic patients who can develop changes in the back of the eye (diabetic retinopathy).
Cataract Surgery
More information on the procedure to remove cataracts
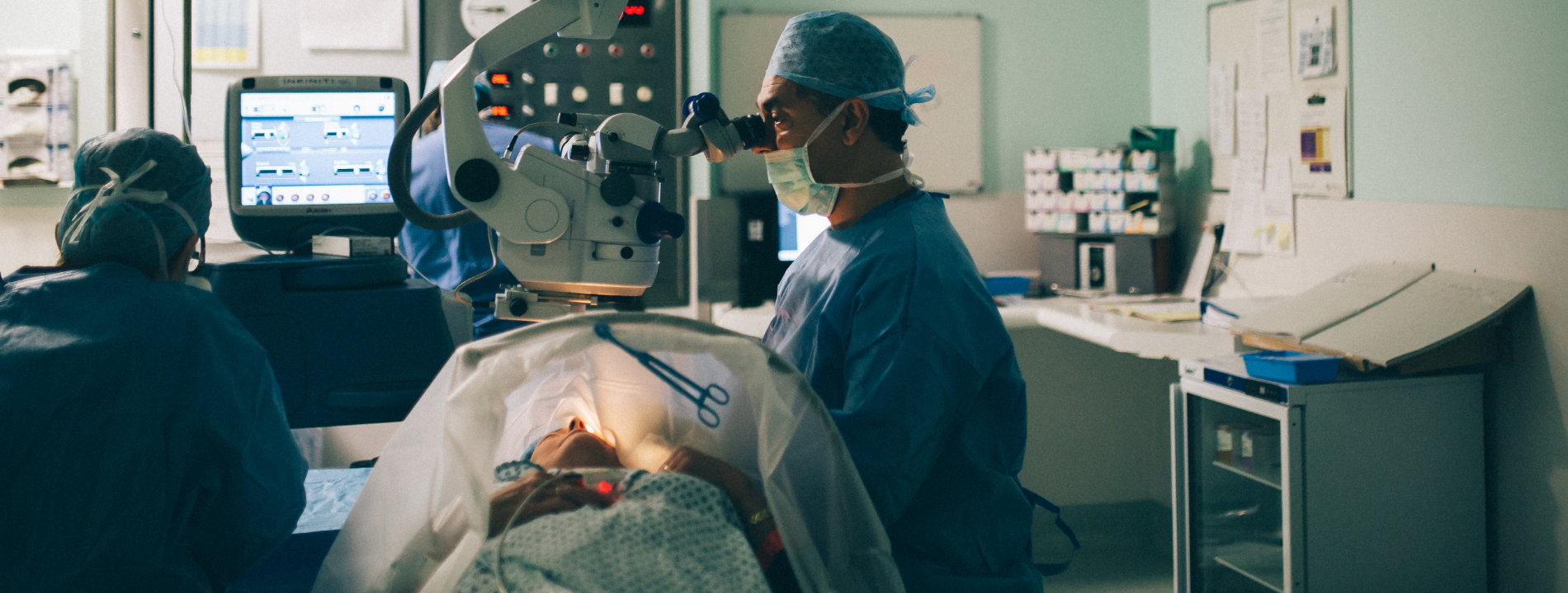
Cataract surgery involves removal of the crystalline lens (cataract) and replacing it with a clear artificial lens implant. It is normally carried out under a local anaesthetic as a daycase procedure with the patient being awake during the surgery.
After the pupil is dilated with eye drops and the eye is anaesthetised, a small (2-2.5 mm) self-sealing incision (opening) is made on the periphery of the cornea. A section of the thin capsular bag enclosing the lens is opened and peeled off. A fine ultrasonic probe is inserted into the eye, through the incision and used to fragment the lens into fine particles, which are simultaneously washed out of the eye. Once all the lens matter is removed an artificial lens is implanted into the empty capsular bag. Normally there is no need to use stitches. The artificial lens can stay in place indefinitely.
What is the risk of cataract surgery?
Whilst cataract surgery has a very high success and satisfaction rate, like any procedure it carries risks. The most serious risks generally relate to complications occurring during surgery (intra-operative) or after surgery (post-operative) which may result in less than desirable visual outcomes and on rare occasions in the loss or deterioration of vision.
Whilst it is imperative that you are aware of these risks and take them in to consideration, as part of making an informed decision, it is important to highlight that the overall risks of cataract surgery remain low for most cases. Please also see the next section.
Will I still need to wear glasses after cataract surgery?
The most common indication for cataract surgery remains the inability to achieve satisfactory vision even with an updated spectacle prescription. Cataract surgery however provides a unique opportunity to try and influence your prescription (refractive outcome). Prior to surgery the surgeon measures the lens implant power required to achieve the desired target, which is discussed and agreed with the patient.
Traditionally the objective is to achieve a visual outcome which renders the individual independent of glasses for distance, but dependent on glasses for near (reading). This is however a personal matter, which you can discuss with your surgeon. Other types of lens implants (multifocal) can offer the benefit of both distance and near vision, although not all candidates will be suitable candidates for these implants.
It is important to realise that despite all efforts and calculations, there are a proportion of patients who may not achieve the expected refractive outcome and may still need to wear spectacles to optimise vision.
Eye Conditions
Mr Hooman Sherafat has over 20 years experience as an ophthalmologist and treats a wide range of eye conditions. Read more.
Book Your Consultation
The first step towards any treatment is a comprehensive consultation with Mr Sherafat. He will go through your concerns and provide you with valuable feedback and a solution to your issue whether it involves surgery or not. You’ll always be in good hands.
Charity Work
Mr Hooman Sherafat has always been actively involved in charity work on an international scale. He has travelled to various developing countries and continues to support charitable eye surgery where he can.


